Table of Contents Show
Do you know what is a molar pregnancy? A molar pregnancy1 is a rare complication noticed by abnormal trophoblast growth that develops into the placenta. It is also a persistent gestational trophoblastic disease or hydatidiform mole.2
During a healthy pregnancy, the placenta grows inside your uterus and provides nutrition to the baby through the umbilical cord. In a molar pregnancy, there is an abnormal tumor growth instead of a placenta.
A molar pregnancy occurs when placental tissue doesn’t develop normally. A tumor forms in the uterus and causes the placenta to become a mass of fluid-filled sacs called grape-like cysts.
This pregnancy doesn’t last long because the placenta cannot provide the nutrition to grow the baby. In rare cases, it may also lead to health risks such as shock and death of the mother.
You can have a molar pregnancy even if you have had a molar pregnancy history. Still, there are quite chances of having a normal pregnancy even after a molar pregnancy.
Molar pregnancies are about 1 in 1000 pregnancies. A molar pregnancy can result in cancer formation that requires early diagnosis and treatment.
1. Complete molar pregnancy vs. partial molar pregnancy
There are two types of molar pregnancy: partial molar pregnancy and complete molar pregnancy. Both kinds are usually benign, but they usually don’t lead to cancer formation in the body’s cells.
In a complete molar pregnancy, there is abnormal and swollen placenta tissue3, and the formation of fluid-filled cysts appears. There’s also no formation of fetal tissue. Only placenta tissue grows in the womb, and the complete molar pregnancy occurs.
When two or more sperm from the father fertilize an unfertilized egg, no fetus forms. The chromosomes from the mother’s egg are inactivated, and the father’s chromosomes are duplicated.
In partial molar pregnancies, there may be abnormally formed placental tissue, but a fetus can be formed but miscarried in early pregnancy. Fetal tissue incompletely forms, but the placenta has no issue. The father led two sets of chromosomes while the mother remained the same, which resulted in 69 embryo chromosomes instead of 46.
2. Causes of Molar Pregnancy
An abnormally fertilized egg may result in gestational trophoblastic disease 4GTD or molar pregnancy. There are 23 pairs of chromosomes in human cells in which; one chromosome from the father and another from the mother.
Anyone can’t control having a molar pregnancy. It can affect all aged women. Mix-ups at the genetic DNA level can lead to molar pregnancy. Most women carry hundreds to thousands of eggs.
Some of these might not form correctly when a defective egg is fertilized by a sperm, resulting in a gene from only the father and no gene from the mother. This leads to molar pregnancy.
In most molar pregnancies, an extra set of chromosomes usually comes from the father. When this happens, a fertilized egg can’t survive and dies a few weeks in early pregnancy.
3. Symptoms of Molar Pregnancy
A molar pregnancy may be noticed as a healthy pregnancy at first. But as time passes, the mother may start to notice some abnormal symptoms other than.
The symptoms of a molar pregnancy include:
3.1. Bleeding:
There is dark brown to bright red vaginal bleeding and tissue clots grape-like cysts during the first trimester (up to 12 weeks).
3.2. Vaginal discharge
Watery brown discharge from your vagina
3.3. Pelvic pain and pressure:
The mother’s stomach may look enlarged even in the early trimester of pregnancy. Abnormal tissue in the placenta grows faster than it should, especially in the second trimester of pregnancy. It can cause pain and abnormal pressure in the uterus.
3.4. Preeclampsia:
A complication in which there is an amount of excess protein in the urine after 20 weeks of pregnancy.
3.5. High HCG levels
The HCG hormone is secreted by the placenta and is one of the pregnancy hormones responsible for nausea and vomiting in pregnant women.
In a molar pregnancy, there may be more abnormal cell growth in the placenta than in healthy pregnancies. Higher HCG levels might lead to more severe nausea and vomiting than healthy pregnancies.
You must consult your doctor if you experience other signs or symptoms of a molar pregnancy. Some other symptoms that doctors may detect in molar pregnancy:
- Anemia(low blood iron)
- Ovarian cysts
- hyperthyroidism
- Nausea and vomiting
4. Risk factors
There are some risk factors for having a molar pregnancy. These may include:
4.1 Maternal age-
This case is more likely to happen in women older than 30 or younger than 20.
4.2 History-
This rare form of pregnancy happens if you’ve had a history of it and a pregnancy loss before. If you’ve had difficulty conceiving, infertility problems, or other pregnancy complications, it can also result in molar pregnancy.
5. How is Molar Pregnancy Diagnosed?
The doctor will recommend blood tests, and scans like MRI and CT scans to confirm the diagnosis of gestational trophoblastic disease if they suspect molar pregnancy.
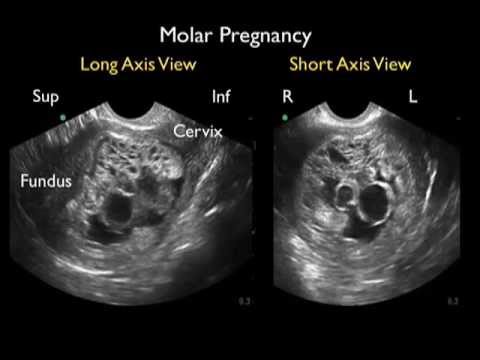
Mainly, this tissue is diagnosed when you go for a normal pregnancy ultrasound scan. In this device, a wand-like device is placed in your vagina and uses sound waves to look inside your uterus.
An ultrasound of a complete molar pregnancy detected as early as eight or nine weeks of pregnancy may show no amniotic fluid, no embryo or fetus, and a thick cystic placenta5. An ultrasound of partial molar pregnancy may show low amniotic fluid and abnormal placenta.
If molar tissues are detected, your doctor will recommend more blood tests to know the level of human chorionic gonadotropin (HCG), a pregnancy hormone, for diagnosis of molar pregnancy. Levels of the hormone HCG increase in pregnancy.
In the case of molar pregnancy, a woman’s HCG level gets higher than it should be in a normal pregnancy.
If your doctors detect a molar pregnancy, they may recommend tests to detect other medical problems, including:
- Preeclampsia
- Hyperthyroidism
- Anemia
6. How is Molar Pregnancy Treated?
A molar pregnancy can’t be as continual as a normal healthy pregnancy. The abnormal placental tissue must be removed to reduce the complications.
With a better treatment plan, you can have a successful pregnancy and a healthy baby again in the future. Molar pregnancies can be successfully treated, and further treatment option includes:
6.1 Dilation and Curettage (D&C)
Your doctor will remove the molar tissue from your uterus with dilation and curettage (D&C) as a treatment. A D&C is done as an outpatient surgery that doesn’t require care in a hospital.
During this procedure, you will receive a general anesthetic, be positioned on your back with your legs in stirrups on the operating room table, and insert a speculum into your vagina to remove tissues.
If you have thought of getting pregnant again, it may be the best treatment option. They widen your cervix and remove molar tissue from the uterus using a vacuum device. It is proven to be the best treatment option in the case of pregnancy loss due to any reason.
After a D&C, your doctor may recommend some blood tests several times to detect whether your HCG levels are returning to normal or not.
6.2 Hysterectomy and Chemotherapy
If there is an increased risk of gestational trophoblastic neoplasia6 (GTN) and if you are no longer desirable for future pregnancies, the uterus may be surgically removed by (hysterectomy).
In rare cases, a complete molar pregnancy can lead to persistent gestational trophoblastic disease (GTD), in which abnormal tissue grows outside your uterus. A D&C is not a good option in this case because it only removes tissue within the uterus. You must need to have a hysterectomy or receive chemotherapy.
In rare cases, molar tissue can reoccur and be cancerous. A molar pregnancy can result in cancer formation such as GTD called choriocarcinoma7, which needs early treatment options such as chemotherapy.
It’s very important to check if there is no molar tissue left behind in your womb. After one molar pregnancy case, the doctor might recommend that you don’t have to conceive for 1 year. After removing your molar tissue, the doctor may ask you for more blood tests and monitoring.
7. Prevention
The only way you won’t have a molar pregnancy is not to get pregnant. Talk to your doctor if you have a history of previously occurring molar pregnancy. You can also ask them about the chances of reoccurrence.
Also, take your opinion on how you are monitored if you get pregnant. There is a higher risk of a complete molar pregnancy than a partial one.
The risk of recurrence of molar pregnancy is quite low, but there is a lower risk for women who have no previous history of molar pregnancy.
8. What is a Molar Pregnancy: Conclusion

Losing a pregnancy is devastating. Give yourself time to grieve and talk about your feelings and allow yourself to experience them fully.
Talk openly to your partner, family, and friends for support. The treatment and the waiting period can also affect your emotional, mental, and physical health.
It’s important to take the time to grieve for any pregnancy loss healthily. Contact and reach out to other women who have gone through such cases. Therapies and counseling can help you look forward to a healthy pregnancy and baby in the not-so-distant future.
9. FAQs
Q. Are molar pregnancies cancerous?
Complete molar pregnancies are usually benign and have no fetal tissue, but they can progress to gestational trophoblastic disease (GTD), a set of conditions that occasionally evolve into cancer. The risk of cancer is lower in partial molar pregnancies since both the placental tissue and some fetal tissue are aberrant.
Q. Is it possible to have a healthy pregnancy after having a molar pregnancy?
Generally speaking, yes. It is advised to wait a while after a molar pregnancy before trying to get pregnant again to give the body time to heal and to carefully watch hCG levels. The majority of women who experience molar pregnancies go on to have subsequent healthy pregnancies.
- Berkowitz, Ross S., and Donald P. Goldstein. “Molar pregnancy.” New England journal of medicine 360.16 (2009): 1639-1645. ↩︎
- CURRY, STEPHEN L., et al. “Hydatidiform mole. Diagnosis, management, and long-term followup of 347 patients.” Obstetrics & Gynecology 45.1 (1975): 1-8. ↩︎
- Benirschke, Kurt. “A review of the pathologic anatomy of the human placenta.” American journal of obstetrics and gynecology 84.11 (1962): 1595-1622. ↩︎
- Seckl, Michael J., Neil J. Sebire, and Ross S. Berkowitz. “Gestational trophoblastic disease.” The Lancet 376.9742 (2010): 717-729. ↩︎
- Fadl, Shaimaa, et al. “Placental imaging: normal appearance with review of pathologic findings.” Radiographics 37.3 (2017): 979-998. ↩︎
- Messerli, Marti L., et al. “Risk factors for gestational trophoblastic neoplasia.” American journal of obstetrics and gynecology 153.3 (1985): 294-300. ↩︎
- Bishop, Bradie N., and Peter F. Edemekong. “Choriocarcinoma.” (2018). ↩︎
Last Updated on by ayeshayusuf