Table of Contents Show
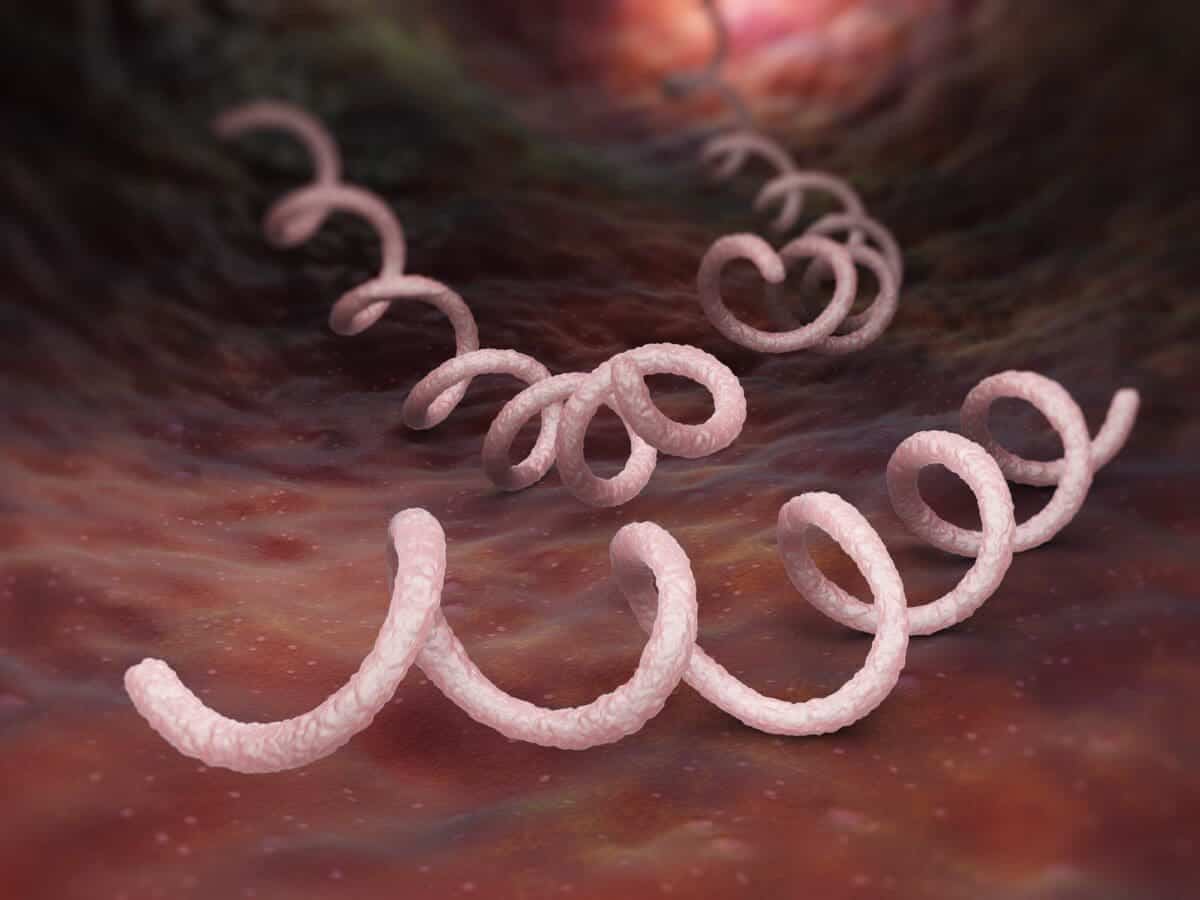
A bacterial infection or treponemal disease called syphilis is a stigmatized disease. It is typically spread through sexual contact like sexual intercourse and leads to the development of sexually transmitted diseases.
The clinical manifestations of the disease typically begin as a painless sore on the mouth, genital ulcers, or sores on the rectum. By touching these sores on the skin or the mucous membranes, syphilis can be transmitted from one person to another.
The sexually transmitted syphilis bacteria can be dormant in the body for decades after the initial infection before coming back to life. Early syphilis can sometimes be cured with a single penicillin injection.
Syphilis1, which is a sexually transmitted disease, can be fatal if left untreated because it can cause serious damage to the heart, brain, or other organs. Mothers can also transmit syphilis to their unborn children.
Symptoms and Types
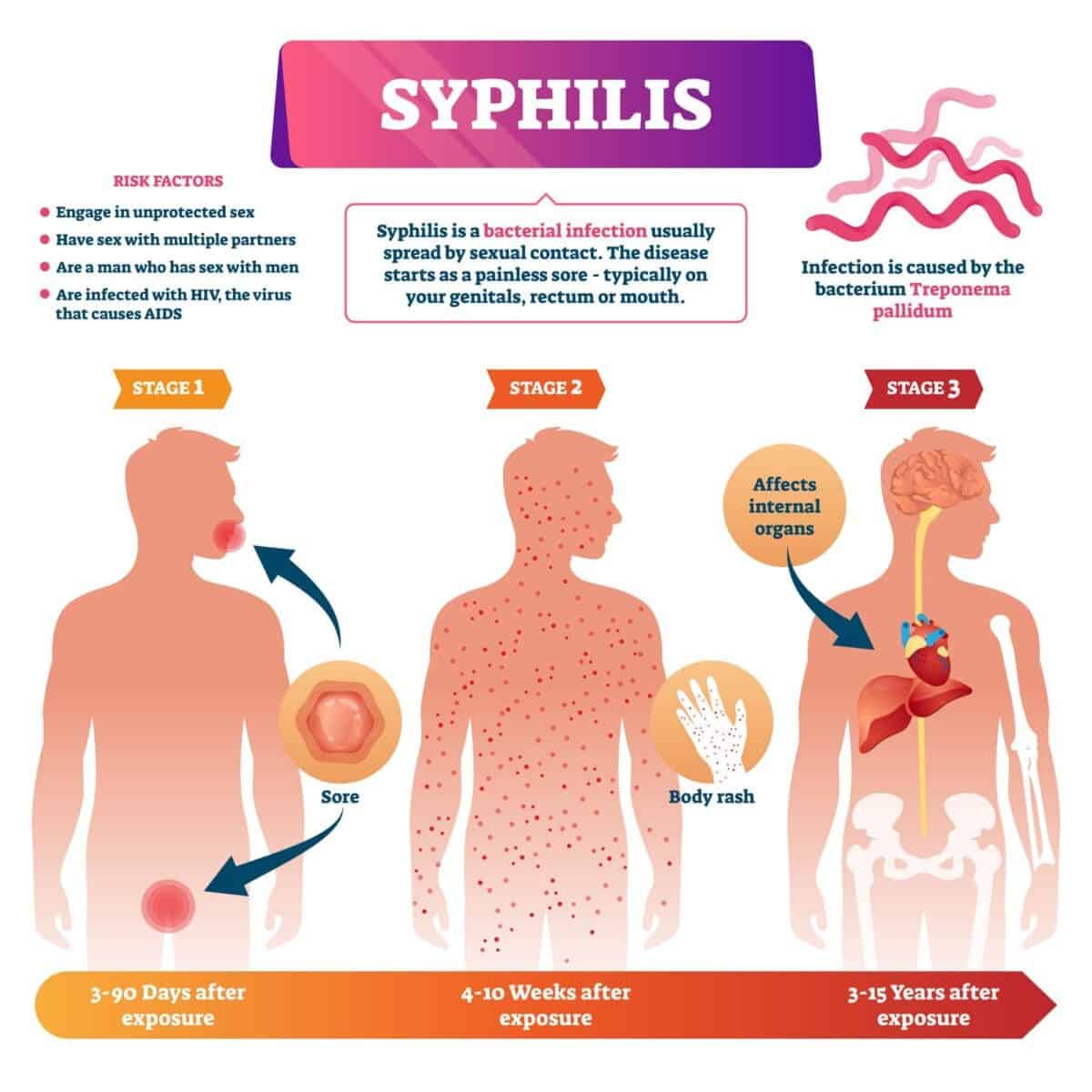
1. Primary syphilis
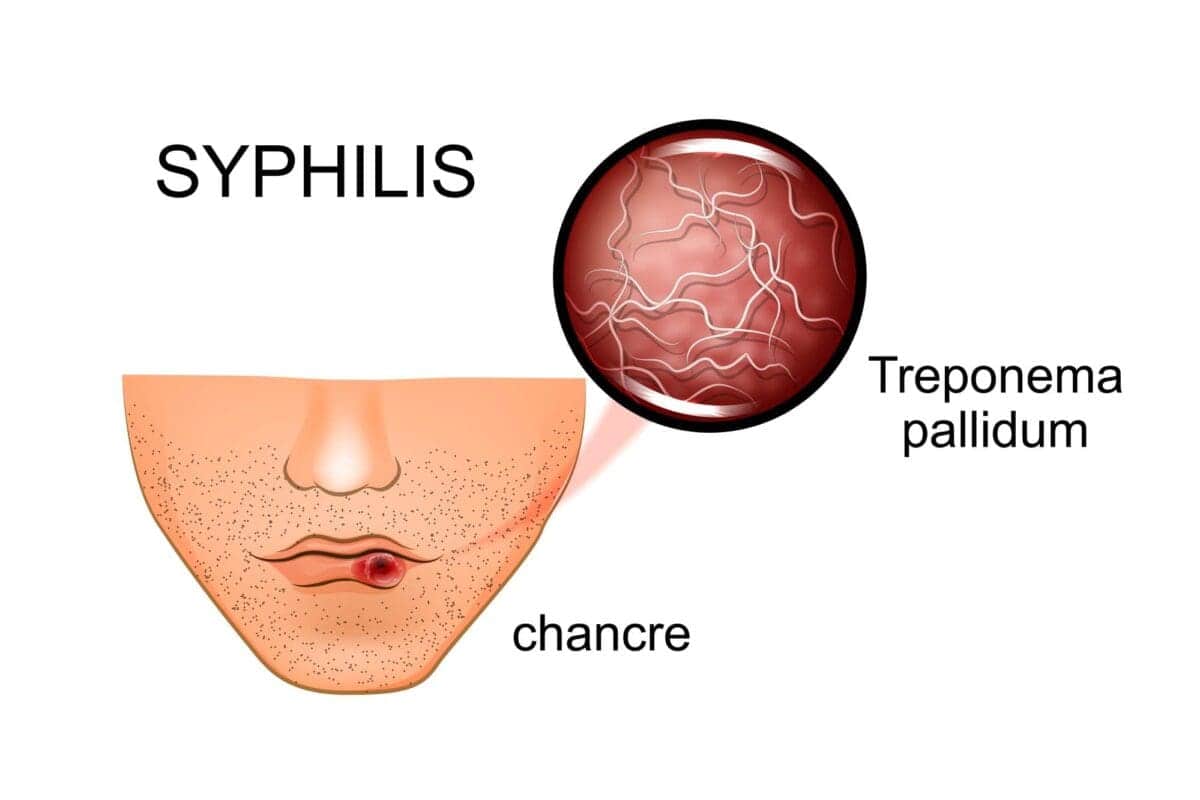
The first sign of syphilis is a chancre (SHANG-kur), which is frequently referred to as a tiny sore. At the site where the germs entered your body because of sexual intercourse, a sore develops. Patients with syphilis often only suffer one chancre but occasionally encounter several.
Typically, the chancre appears three weeks after exposure. Because the chancre is typically painless and can be concealed within the vagina or rectum, many persons with syphilis fail to discover their condition. The wound naturally heals within three to six weeks.
2. Secondary syphilis
A few weeks after the initial chancre heals, secondary syphilis may manifest as a rash that begins on your torso and then spreads to cover your entire body, including the palms of your hands and the soles of your feet.
Usually not itchy, this rash may also be accompanied by lesions that resemble warts in the mouth or genitalia. Some individuals also experience hair loss, muscle aches, fevers, sore throats, and swollen lymph nodes.
These secondary syphilis warning signs and symptoms may go away in a few weeks or come back for up to a year.
3. Latent syphilis
There are no outward indications or symptoms of syphilis during the latent (hidden) stage of the disease. Despite the absence of any symptoms or signs, syphilis will continue to exist in the body without treatment. Early latent syphilis is syphilis that has been latent for less than a year. Syphilis that has been latent for longer than 12 months is referred to as late latent syphilis.
When there are insufficient alternative diagnoses that can be made or evidence to establish that the initial infection occurred within the previous year, latent syphilis of undetermined duration results for years, syphilis can remain latent.
4. Congenital syphilis
Treponema pallidum, a multisystem infection, causes congenital syphilis or venereal diseases, which are passed from mother to fetus through the placenta.
The clinical manifestations include typical skin lesions, lymphadenopathy, hepatosplenomegaly, failure to feed, bloody nasal discharge, perioral fissures, meningitis, choroiditis, hydrocephalus, seizures, intellectual impairment, osteochondritis, and pseudoparalysis (newborn parrot atrophy) are early warning indications in congenital syphilis spread by treponema pallidum.
Later symptoms include dental abnormalities, periosteal lesions, paresthesia, tabes, optic atrophy, interstitial keratitis, and gummatous ulcers.
The clinical diagnosis is supported by microscopy or serology. Penicillin is used as a remedy in congenital syphilis treatment to fight treponema pallidum.
5. Tertiary syphilis
Untreated syphilis patients typically do not progress to get tertiary syphilis. When it does occur, it may, nevertheless, have an impact on a variety of organ systems and cause infectious diseases. These include the neurological system, the brain, and the heart and blood arteries.
It is an extremely dangerous infection that can develop 10 to 30 years after your initial infection. The disease destroys your internal organs and can be fatal in tertiary syphilis. Tertiary syphilis in a patient usually has to be detected using a number of tests.
Neurosyphilis, Ocular syphilis, and Otosyphilis

Syphilis can spread to the eye (ocular syphilis), the brain and neurological system (neurosyphilis), or the ear (otosyphilis) if it is not treated. This could occur at any of the aforementioned stages.
- Neurosyphilis symptoms and signs can include severe headache, muscle weakness, or trouble moving your muscles, changes in personality or dementia (issues with memory, thinking, or decision-making), as well as mental changes such as difficulty focusing, disorientation, or personality changes.
- Ocular syphilis symptoms and signs can include eye discomfort and/or redness, vision abnormalities, or even blindness.
- Otosyphilis symptoms and signs can include tinnitus, hearing loss, vertigo, ringing, buzzing, roaring, or hissing in the ears.
How did Syphilis Start?
The origin of syphilis can be traced back to the Columbian hypothesis, which has had the most world pre-Columbian evidence behind it. It contests that sailors who traveled to America with Christopher Columbus for the first time in 1492 returned to Europe with venereal disease.
The first outbreak among the French troops in Europe during the War of Naples or the European syphilis epidemic in 1495 coincidentally occurred at the same time as this occurrence. Furthermore, there is evidence that suggests syphilis or treponemal disease existed in the New World at the time of Christopher Columbus’s arrival.
The treponemal disease appears to have been a more severe condition when it initially spread to Europe in the 15th century than it is now. Based on texts, medical literature, and artwork from that era, the venereal disease appears to have spread and killed its victims more quickly in that period.

Syphilis was a relatively new disease in Europe at the time, and people did not yet have immunity to it, which is why some researchers believe it was particularly brutal in those early years. Because of its painful and revolting symptoms, syphilis was referred to as “the great pox” in the 15th century.
Treatment options at the time were limited and unsuccessful. Some of the mercury treatments used by doctors to treat patients’ ailments were extremely painful and even fatal, frequently leading to mercury poisoning.
Recent studies on the Columbian hypothesis and other works have attempted to explain the origins and early history of syphilis along with the global spread of the disease using a combination of genetic analysis and data about pathogenic human treponemal diseases, paleopathological diagnosis and evidence discovered through carbon dating, and analysis of bone pathology.
The origin of endemic syphilis or new disease on the basis of genomic, morphological, and serological characteristics of the etiologic agents of human treponematoses are similar.
Their genome sizes are nearly identical at roughly 1.14 Mbp. Based on the complete genome sequence and DNA-DNA hybridization tests, these organisms might have shared a common ancestor that was clonal in origin and closely related.
A study that combined a global map of paleopathological diagnosis and dental evidence with evolutionary models based on genetic analysis of Treponema species worldwide supported the Columbian hypothesis.
It suggests that Treponema Pallidum originated in the Old World as a non-venereal infection or non-venereal syphilis before spreading to the Middle East and Eastern European endemic syphilis and then to America, taking the form of New World yaws.
It’s likely that a treponema pallidum strain from the Americas underwent genetic changes and was reintroduced into the Old World, where it gave rise to the ancestor of the treponemal disease or treponemal infection, treponemal pallidum strain that causes syphilis and distinct diseases.
The pre columbian evidence and Columbian hypothesis are supported by a more recent study that used genome sequencing to show that treponemal pallidum isolates obtained from syphilis patients in 13 countries across Europe, the Americas, and Asia all shared a common ancestor that lived only after the 15th century.
As was previously established, there was basically no conclusive proof that endemic syphilis occurred in the Old World before the 1500s. Even in ancient Chinese manuscripts, where descriptions of many Old World diseases have been uncovered, there has never been a clear mention of syphilis previously.
The Italians started a blame game, which led to the term “The French Disease” or French pox. The treponemal diseases spread rapidly throughout Europe, causing devastating illnesses and infectious diseases.
Like Squillaci, people in early modern European regions that are today known as Germany and the United Kingdom once referred to syphilis as “the French disease.” Syphilis was referred to in France as “the Neapolitan disease,” i.e., originating in Naples, Italy.
While Poles refer to it as “the German disease,” Russians refer to it as “the Polish disease.” In the past, Turks referred to syphilis as “the Christian disease,” while Muslims attributed it to Hindus. In reality, very few groups have ever been held accountable for spreading the treponemal disease.
Syphilis existed in the New World when Columbus first arrived there. Documentation of syphilis in the Dominican Republic, where he really landed, is particularly significant.
6%–14% of the skeletal remains from the El Soco (800 A.D.), Juan Dolio (1400 A.D.), La Caleta (1200–1300 A.D.), Atajadizo (1200–1300 A.D., and Cueva Cabrera (1200–1300 A.D.) sites exhibit the periosteal reaction typical of syphilis. Between 1.7 and 2.6 bone groups on average were impacted, which caused bone destruction.
The remodeling of the saber shin was frequently so severe as to cover up any periosteal response surface signs completely. The skeletal evidence proves that syphilis existed in the Dominican Republic, where Christopher Columbus first set foot. Columbus’ crew had the opportunity and resources to enter into a contract and spread venereal syphilis.
The research found that it was not Columbus’ fault. Armelagos and his coworkers carefully examined all the information in these earlier papers. They discovered that the majority of the skeletal material didn’t truly fulfill at least one of the common diagnostic criteria for chronic syphilis, such as pitting and swelling of the long bones and caries sicca on the skull.
Intriguingly, the history of syphilis and its effects in the Old World in the first century appeared to advance more quickly and cause more severe morbidity and death than the version of the illness that was recorded from the 16th century onward. It’s conceivable that this less serious, slowly spreading form of syphilis gave rise to the most prevalent venereal diseases on the entire planet.
Literary Record
The term “syphilis” itself comes from a legend about a shepherd by the name of Syphilis. Girolamo Frasastoro came up with the term “syphilis sive morbus gallicus” in 1530. The phrase “great pox” emerged as a way to distinguish the illness from smallpox due to the associated rash (pox).
Even though the phrase has been in use for two centuries, syphilis quickly became a social disgrace, leading to different attributions: The term “French pox” was used by the Germans and the English, “the Polish sickness2” by the Russians, “the German sickness” by the Poles, “the Neapolitan sickness” by the French, “the Neapolitan sickness.”
The Japanese referred to “the Canton rash” or “the Chinese ulcer,” whereas the Flemish, Dutch, Portuguese, and North Africans referred to “the Spanish sickness” or “the Castillian sickness.”
It’s intriguing how closely the history of syphilis and literature are related. The poem “Syphilis, Sive Morbus Gallicus” (“Syphilis, or the French Disease”) by Italian physician-poet Girolamo Fracastoro in 1530 served as the inspiration for the disease’s name.
The poem narrates the tale of a shepherd named Syphilus who, after blaming and insulting the Sun God for the drought that had killed off his flocks, was punished by the gods by contracting this horrifying illness.
The disease was significantly more severe than current venereal syphilis during the first century following the first known syphilis outbreak in the Old World in 1495. The treponemal disease, which was much more terrible than contemporary venereal syphilis, motivated numerous writers and poets to express their anguish via their works.
First Syphilis Treatment
Early on in the 16th century, syphilis treatments included barbers and wound surgeons who were primarily responsible for administering guaiacum, or holy wood, and mercury skin inunctions or ointments, also known as mercury treatment, as remedies to cure syphilis and infectious diseases.
It was believed that using a sweat bath on the infected person would cause salivation and that sweating would remove the syphilitic toxins.
As a result of the dreadful side effects of mercury, which included neuropathies, kidney failure, severe mouth ulcers, and tooth loss, many people perished from mercury poisoning as opposed to the actual disease. Typically, a course of treatment would last years.
The corrosive sublimate, also known as mercuric chloride or liquid Swietenii, was first used internally as internal medicine by Austrian army surgeon Gerhard van Swieten (1700–1772) to cure syphilis.
Guido Bacelli later synthesized the substance as an injectable in 1894. Calomel3, a purgative and laxative used as an injunction, a tablet, and later as an injection, was popular in the late 19th century.
The Australian Pharmaceutical Formulary still contained the pharmaceutical formulae for unguentum hydrargyri ammoniate and unguentum hydrargyri salicylate in 1955. Ammoniated and salicylated mercury ointments were also created.
Mercury remained popular as a syphilis therapy up until 1910, when Ehrlich found that arsenic had anti-syphilitic properties and created Salvarsan, also known as the “magic bullet.”
Discoveries of syphilis treatment
Physicians started looking for alternatives to treating syphilis when they found that mercury’s hazardous effects frequently overshadowed any potential advantages. The elixir Decoctum Zittmani4 was created by the Polish surgeon-general Friedrich Zittman (1671–1757) and contained sarsaparilla root with traces of mercury.
Iodine therapy, or potassium iodide with low doses of mercury, was first introduced by English surgeon William Wallace (1791-1837). In the late 19th century, many other metals, including tellurium, vanadium5, platinum, and gold, were attempted, but all proved ineffective.
Fritz Richard Schaudinn, a German naturalist, and Erich Hoffmann, a dermatologist, identified the causative organism of syphilis-causing bacteria Spirochaeta pallida (now known as Treponema pallidum), which was spiral-shaped and white when illuminated by darkness on the ground.
In 1917, Julius Wagner-Jauregg, an Austrian doctor, developed fever therapy for the treatment of neurosyphilis by giving the patient malaria and then treating the malaria with quinine.
It had been noted that neurosyphilis symptoms improved after a febrile illness, and the theory was that quinine, which is used to treat malaria, was more effective against syphilis than mercury or arsenic.
In order to treat syphilis and gonorrhea, two American doctors named Fred A. Kislig and Walter M. Simpson developed the electropyrexia 5treatment in 1936. They did this by employing short-wave equipment to cause pyrexia in a patient.
A theoretical and practical approach by John Mahoney, Richard Arnold, and AD Harris, penicillin was first used to treat syphilis in 1943. Four patients with primary syphilis chancres were treated by Mahoney and his coworkers at the US Marine Hospital in Staten Island with intramuscular injections6 of penicillin four hours a day for eight days in total, curing the syphilis.
This was a turning point in the treatment of syphilis since it was discovered that penicillin7, when given during either its primary or secondary stages, was extremely successful and had few adverse effects compared to mercury or arsenic8.
For more such related articles, click here.
- Goh, B. “Syphilis in adults.” Sexually transmitted infections 81.6 (2005): 448. ↩︎
- Kotowska, Maja, et al. “Awareness of endometriosis symptoms—a cross sectional survey among Polish women.” International Journal of Environmental Research and Public Health 18.18 (2021): 9919. ↩︎
- Gliozzo, Elisabetta. “Pigments—Mercury-based red (cinnabar-vermilion) and white (calomel) and their degradation products.” Archaeological and Anthropological Sciences 13.11 (2021): 210. ↩︎
- Koniewicz, Krzysztof Andrzej, and Monika Urbanik. “Z manuału Ignacego Łukasiewicza.” Farmacja Polska 78.3 (2022). ↩︎
- Isler, Madeleine F., et al. “Syphilitic Folliculitis: A Case Report With Demonstration of Spirochetes Showing Follicular Epitheliotropism.” The American Journal of Dermatopathology 44.11 (2022): 837-839. ↩︎
- Nowak, Zuzanna, et al. “Intramuscular Injections and Dry Needling within Masticatory Muscles in Management of Myofascial Pain. Systematic Review of Clinical Trials.” International Journal of Environmental Research and Public Health 18.18 (2021): 9552. ↩︎
- Stone Jr, Cosby A., et al. “The challenge of de‐labeling penicillin allergy.” Allergy 75.2 (2020): 273-288. ↩︎
- Rahaman, Md Shiblur, et al. “Environmental arsenic exposure and its contribution to human diseases, toxicity mechanism and management.” Environmental Pollution 289 (2021): 117940. ↩︎
Last Updated on by Sathi Chakraborty, MSc Biology